Nursing Management for Peritonitis
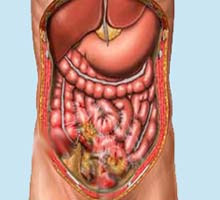
Peritonitis is an inflammation of the membrane which lines the inside of the abdomen and all of the internal organs. This membrane is called the peritoneum.
Causes of peritonitis
Most often, peritonitis is caused by the introduction of an infection from a perforation of the bowel such as a ruptured appendix or diverticulum. Other sources include perforations of the stomach, intestine, gallbladder, or appendix. Pelvic inflammatory disease in women is also a common cause of peritonitis. Peritonitis can also develop after surgery if bacteria enters into the abdomen during an operation.
Signs and Symptoms of Peritonitis
The signs and symptoms of peritonitis include:
- Swelling and tenderness in the abdomen with pain ranging from dull aches to severe, sharp pain
- Fever and chills
- Loss of appetite
- Thirst
- Nausea and vomiting
- Reduced urine output
- Not being able to pass gas or stool
The following factors may increase the risk for primary peritonitis:
- Liver disease (cirrhosis)
- Fluid in the abdomen
- Weakened immune system
- Pelvic inflammatory disease
- Risk factors for secondary peritonitis include:
- Appendicitis (inflammation of the appendix)
- Stomach ulcers
- Torn or twisted intestine
- Pancreatitis
- Inflammatory bowel disease, such as Crohn's disease or ulcerative colitis
- Injury caused by an operation
- Peritoneal dialysis
- Trauma
Prevention of Peritonitis
There is no way to prevent peritonitis, since the diseases it accompanies are usually not under the voluntary control of an individual. However, prompt treatment can prevent complications.
Treatment of Peritonitis
Treatment depends on the source of the peritonitis, but an emergency laparotomy is usually performed. Any perforated or damaged organ is usually repaired at this time. If a clear diagnosis of pelvic inflammatory disease or pancreatitis can be made, however, surgery is not usually performed. Peritonitis from any cause is treated with antibiotics given through a needle in the vein, along with fluids to prevent dehydration.
Nursing Management for Peritonitis
Replacement fluids, colloids and electrolytes is the main focus. Given analgesics to manage pain, antiemetics can be given as a treatment for nausea and vomiting. Oxygen therapy by nasal cannula or mask will improve oxygenation is adequate, but sometimes the incubation shape of the airway and ventilation is required. But medical nonoperatif using antibiotic therapy, hemodynamic therapy is used for lung and kidney, metabolic and nutritional therapies and therapeutic modulation of the inflammatory response.
Management of penetrating trauma patients with hemodynamically stable at the lower chest or abdomen vary, but all surgeons agree patients with signs of peritonitis or hypovolemia should undergo surgical exploration, but it is uncertain for patients with no signs of sepsis-with stable hemodynamics. All stab wounds to the chest and abdomen should be explored first. When a penetrating wound peritoneum, the action required laparotomy. Prolapsed viscera, signs of peritonitis, shock, loss of bowel sounds, there is blood in the stomach, bladder and rectum, the presence of intraperitoneal free air and a positive peritoneal lavase also an indication perform laparotomy. If not, patients should be observed for 24-48 hours. While the gunshot wound patients are encouraged to laparotomy.
Perioperative nursing is a term used to describe a variety of nursing functions related to the surgical patient experience that includes three phases:
1. Preoperative phase of perioperative nursing role begins when a decision for surgical intervention is made and ends when the patient is being led shirt surgery. The scope of nursing activities during this time may include establishing a basic assessment of the patient in the clinic or at home, underwent preoperative interview and prepare patients for surgery and anesthesia given. However, the nursing activities may be limited to assessing the patient's preoperative place operating room.
2. Intraoperative phase of the perioperative nursing begins when the patient entered or transferred or assigned to the recovery chamber. In this phase the scope of nursing activities may include: installing infusion (IV), providing intravenous medication, conduct a thorough physiological monitoring during surgical procedures and maintaining patient safety. In some instances, nursing activities limited to grasp the hands of patients during induction of general anesthesia, acting in its role as a nurse scub, or assist in positioning the patient on the operating table by using the basic principles of body alignment.
3. Postoperative phase, beginning with the inclusion of patient recovery chamber and ends with follow-up evaluation in the framework of the clinic or at home. The scope of nursing includes a wide range of activities during this period. In the immediate postoperative phase, the focus on assessing the effects of anesthetic agents and monitoring of vital functions and prevent complications. Nursing activity then focuses on healing patients and do counseling, follow-up care and referrals are essential for a successful recovery and rehabilitation followed by repatriation. Each phase are reviewed in detail in this unit. When relevant and possible, the nursing process of assessment, nursing diagnosis, intervention and evaluation are described.
ads
0 komentar:
Post a Comment